Fatty Liver Alert: 5 Warning Signs You Need a Liver Detox Immediately
Hook: Did you know that nearly 25% of adults worldwide are walking around with a silent metabolic time bomb in their abdomen? Fatty liver disease has become a global epidemic, yet it rarely screams for attention until significant damage has occurred.
Problem: Most people ignore early warning signs like brain fog, stubborn belly fat, or persistent fatigue, assuming they’re just “getting older” or “eating a bit too much.” But when your liver’s natural filtration system becomes overwhelmed, these aren’t minor inconveniences—they’re your body’s red flags.
Promise: In this guide, we’ll uncover the 5 critical signs that indicate your liver needs urgent support, break down the science behind metabolic liver stress, and share expert-backed liver detox strategies that actually work. No extreme cleanses. No dangerous shortcuts. Just science, simplicity, and sustainable health.
🔍 Quick Answer
Common signs that you may need urgent fatty liver support include persistent fatigue, unexplained belly fat, brain fog, digestive bloating, and right-side abdominal discomfort. These symptoms often indicate metabolic stress, inflammation, and impaired liver function. Supporting your liver early with targeted nutrition, reduced sugar intake, and movement can significantly improve hepatic health.
📖 Sommaire (Table of Contents)
- What Is Fatty Liver Disease?
- Why Your Liver Detox Pathways Matter
- 5 Signs You Need an Urgent Liver Detox Right Now
- Hidden Causes Behind Fatty Liver Disease
- Best Natural Liver Detox Strategies
- Foods That Help Reverse Fatty Liver Naturally
- Can Fatty Liver Be Reversed?
- Common Mistakes & Myths
- Frequently Asked Questions
What Is Fatty Liver Disease?
Understanding NAFLD and Liver Fat Accumulation
Non-alcoholic fatty liver disease (NAFLD) occurs when excess fat builds up in liver cells, unrelated to heavy alcohol consumption. It ranges from simple steatosis (fat accumulation without inflammation) to non-alcoholic steatohepatitis (NASH), which involves liver cell damage and fibrosis. According to the Mayo Clinic, NAFLD is closely tied to metabolic syndrome, insulin resistance, and visceral obesity.
Why Fatty Liver Often Goes Undetected
The liver is remarkably resilient. It can function even when up to 70% of its tissue is compromised. This silent progression means early-stage fatty liver rarely causes noticeable symptoms. Without routine blood work or imaging, metabolic liver dysfunction can quietly advance for years. Early screening and lifestyle awareness are your best defenses.
Why Your Liver Detox Pathways Matter
The Liver’s Natural Detoxification System
Your liver doesn’t need “miracle cleanses” to work—it needs the right nutrients to run its built-in two-phase detox pathway:
- Phase I (Cytochrome P450): Breaks down toxins, medications, and hormones into intermediate compounds.
- Phase II (Conjugation): Neutralizes those intermediates so they can be safely excreted via bile or urine.
When Phase I runs faster than Phase II, oxidative stress and inflammation spike, overwhelming liver cells and accelerating fat storage.
What Overloads the Liver
Modern lifestyles constantly stress hepatic function. Primary overload drivers include:
- Ultra-processed foods and hidden seed oils
- Excess fructose and refined sugars
- Sedentary behavior and poor sleep quality
- Environmental toxins and chronic low-grade inflammation
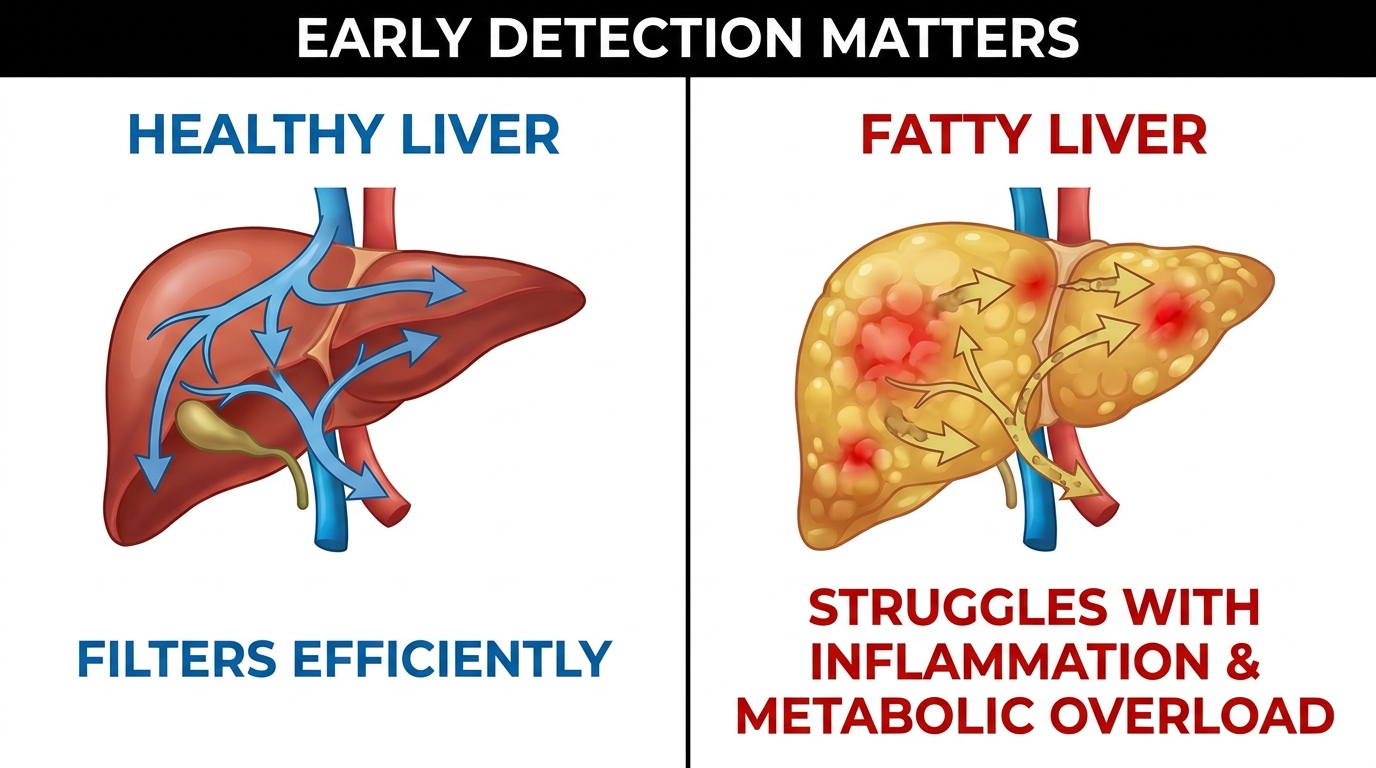
Early detection matters: A healthy liver filters efficiently, while a fatty liver struggles with inflammation and metabolic overload.
5 Signs You Need an Urgent Liver Detox Right Now
1. Persistent Fatigue and Low Energy
If you’re sleeping enough but still feel drained by 2 PM, your liver may be struggling to regulate blood sugar and clear metabolic waste. Hepatic inflammation impairs mitochondrial function, leading to cellular energy deficits.
2. Belly Fat and Rapid Weight Gain
Visceral fat around the midsection isn’t just cosmetic—it’s a direct marker of insulin resistance and hepatic lipotoxicity. When the liver can’t process fats efficiently, it stores them locally, creating a stubborn “spare tire” that resists dieting.
3. Brain Fog and Poor Concentration
The gut-liver-brain axis is real. When toxin clearance slows, inflammatory cytokines cross the blood-brain barrier, disrupting neurotransmitter balance. Patients often report “mental cloudiness,” irritability, and difficulty focusing.
4. Digestive Problems and Bloating
The liver produces bile, essential for fat digestion and gut microbiome balance. Impaired bile flow leads to bloating, irregular bowel movements, and food sensitivities. Supporting fatty liver detox pathways often restores digestive comfort within weeks.
5. Elevated Liver Enzymes or Right-Side Abdominal Pain
ALT and AST elevations on blood tests signal hepatocyte stress. Dull aching under the right rib cage may indicate liver enlargement. These are clinical red flags that warrant immediate lifestyle adjustment and medical consultation.
Hidden Causes Behind Fatty Liver Disease
- Insulin Resistance: The root driver of hepatic fat storage. When cells resist insulin, the liver converts excess glucose into triglycerides.
- Excess Sugar & Fructose: Fructose is metabolized almost entirely in the liver. High intake directly fuels de novo lipogenesis.
- Chronic Inflammation: Low-grade systemic inflammation accelerates liver fibrosis and impairs Phase II detox pathways.
- Sleep Deprivation & Stress: Cortisol spikes disrupt glucose metabolism and promote visceral fat deposition.
- Sedentary Lifestyle: Muscle inactivity reduces glucose uptake, forcing the liver to handle excess metabolic load.
Best Natural Liver Detox Strategies for Fatty Liver
Adopt a Liver-Friendly Diet
Focus on a Mediterranean-style framework: high fiber, abundant cruciferous vegetables, omega-3-rich fish, and monounsaturated fats. Research from NIH-funded studies confirms that dietary pattern shifts significantly reduce hepatic fat content.
Reduce Sugar and Ultra-Processed Foods
Eliminate sugary beverages, hidden fructose, and refined carbs. These are the primary fuel sources for liver fat accumulation. Swapping to whole-food carbohydrates stabilizes insulin and reduces hepatic workload.
Support Glutathione Production
Glutathione is the liver’s master antioxidant. Boost it naturally with sulfur-rich foods like garlic, onions, broccoli, and whey protein (if tolerated). Adequate glutathione ensures Phase II detox runs efficiently.
Exercise for Liver Fat Reduction
Both aerobic and resistance training improve insulin sensitivity and mobilize liver fat. Aim for 150 minutes of moderate activity weekly, plus 2 strength sessions. Even brisk walking triggers meaningful metabolic improvements.
Improve Sleep and Stress Management
Prioritize 7–8 hours of quality sleep. Implement stress-reduction techniques like diaphragmatic breathing, mindfulness, or evening walks. Lower cortisol = better liver function.
👉 Want to support your liver the right way?
Get your FREE 7-Day Liver Detox Guide with simple, science-backed steps you can start today.
- ✅ Easy daily plan
- ✅ Proven liver-support foods
- ✅ No extreme detox or dangerous methods

Nature’s pharmacy: Whole, nutrient-dense foods provide the cofactors your liver needs to repair and regenerate.
Foods That Help Reverse Fatty Liver Naturally
✅ Best Foods
- Avocados: Rich in glutathione precursors and healthy monounsaturated fats.
- Leafy Greens: High in chlorophyll, which binds environmental toxins.
- Fatty Fish (Salmon, Sardines): Omega-3s reduce hepatic inflammation and triglycerides.
- Extra Virgin Olive Oil: Improves insulin sensitivity and reduces liver fat accumulation.
- Green Tea: Catechins (EGCG) directly support hepatic fat oxidation.
- Berries & Walnuts: Antioxidant powerhouses that combat oxidative stress.
❌ Foods to Avoid
- Sugary drinks and fruit juices (fructose overload)
- Processed carbs and refined flours
- Fried foods and industrial seed oils
- Excess alcohol (even moderate intake strains a compromised liver)
Can Fatty Liver Be Reversed?
What Research Says
Absolutely. The liver is the only organ capable of significant self-regeneration. Studies published in Cleveland Clinic resources show that a 7–10% reduction in body weight, combined with dietary changes, can reverse early-stage NAFLD in 3–6 months. Consistency beats intensity.
When to See a Doctor
Consult a healthcare provider if you experience:
- Persistent right-upper quadrant pain
- Jaundice (yellowing of skin/eyes)
- Unexplained swelling in legs or abdomen
- Consistently elevated liver enzymes despite lifestyle changes
Common Mistakes & Myths
- Myth: “Juice cleanses detox the liver.” Fact: Extreme fasting spikes cortisol and can worsen fat mobilization stress. The liver detoxifies best with steady nutrition, not starvation.
- Myth: “Only alcoholics get fatty liver.” Fact: NAFLD is primarily metabolic, driven by sugar, insulin resistance, and lifestyle—not just alcohol.
- Mistake: Ignoring sleep and stress. Hepatic repair peaks during deep sleep. Poor rest sabotages even the cleanest diet.
- Mistake: Relying on unverified supplements. Many “liver detox” pills lack clinical backing and may interact with medications. Always prioritize food-first strategies.
Frequently Asked Questions
Early signs often include unexplained fatigue, mild right-side abdominal discomfort, brain fog, bloating after meals, and stubborn belly fat. Many people have no symptoms initially, which is why routine blood work (ALT/AST) is crucial for early detection.
There’s no fixed timeline, but most people notice improved energy and digestion within 2–4 weeks of consistent lifestyle changes. Significant hepatic fat reduction typically occurs over 3–6 months with sustained dietary adjustments, regular movement, and adequate sleep.
Hydration supports kidney function and bile flow, which indirectly aids liver detoxification. However, water alone doesn’t “flush” fat from the liver. True hepatic recovery requires reducing metabolic overload through nutrition, reducing fructose, and improving insulin sensitivity.
The most effective approach combines: (1) eliminating added sugars and refined carbs, (2) increasing omega-3 and fiber intake, (3) engaging in 150+ minutes of weekly exercise, and (4) prioritizing 7–8 hours of sleep. Crash diets backfire; sustainable metabolic shifts yield lasting results.
If left unaddressed, fatty liver can progress to NASH, fibrosis, cirrhosis, or liver cancer. However, in its early stages, it’s highly reversible. The key is early intervention through evidence-based nutrition and lifestyle modifications.
Whole foods should always be your foundation. Some supplements like milk thistle, NAC, or berberine show promise in clinical studies, but they aren’t magic bullets. Always consult a healthcare provider before starting supplements, especially if you take medications or have existing liver conditions.
🔵 Ready to take your liver health to the next level?
Join our VIP 7-Day Liver Detox Program and follow a complete, structured system designed for real results.
- ✔ Step-by-step detox protocol
- ✔ Nutrition + lifestyle guidance
- ✔ Designed for safe, effective liver support
Conclusion
Fatty liver disease doesn’t have to be a life sentence. With early awareness, strategic nutrition, consistent movement, and stress management, your liver can heal, regenerate, and return to optimal function. The warning signs are your body’s way of asking for support—listen to them before progression occurs.
Start today. Swap one processed meal for whole foods. Take a 20-minute walk. Prioritize sleep. Small, consistent actions compound into profound metabolic transformation. Your liver works tirelessly for you—give it the tools it deserves.

What if your fatigue, brain fog, and digestive issues weren’t “normal”… but a sign your body is overloaded and needs a reset?
“Your liver controls more of your health than you think. That discovery changed everything.”
For years, Achraf Mojih lived exactly that reality — constant low energy, poor digestion, and a feeling that something just wasn’t right. His journey from chronic fatigue to vibrant health led him to discover the powerful role of liver function in overall wellness.
Credentials & Expertise
Clinical Experience


